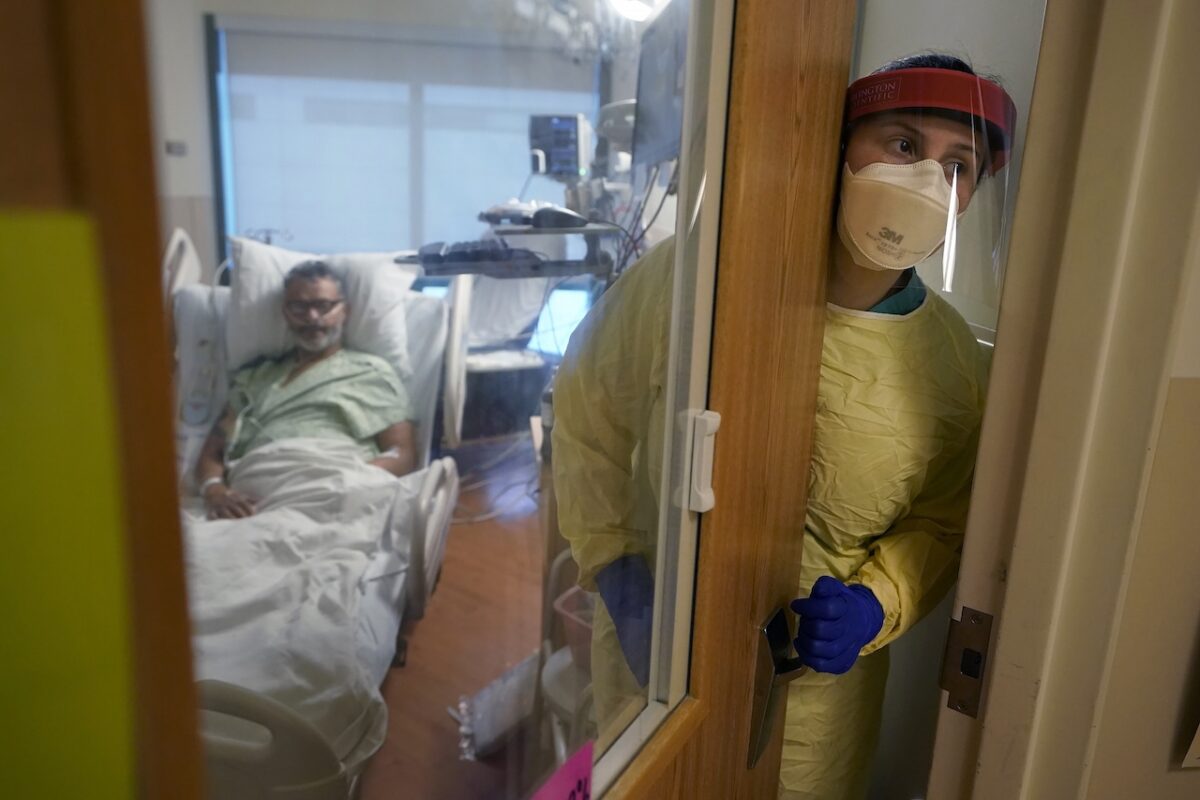
A New Hampshire nurse during the COVID-19 pandemic. The pandemic is over, but the burnout remains. (AP Photo/Steven Senne, File)
Medicaid cuts could worsen an existing nursing shortage that is already exhausting nurses and putting patients in danger.
[This story is part of Cardinal & Pine’s “Bad Medicine” series, a wide-ranging look at how new federal healthcare policies threaten to overwhelm already overwhelmed doctors and nurses, widen health disparities in rural areas, and make North Carolinians sicker. For more of Bad Medicine, tap here.]
It’s a crucial equation for quality healthcare in North Carolina, but the math just doesn’t add up: Though the demand for health care is increasing as the population ages, the state does not have enough nurses to meet it.
North Carolina’s senior population is expected to double in the next 20 years, and heart disease and other chronic conditions are already the leading causes of death in most counties. The effects of the COVID-19 pandemic also continue to reverberate, while falling vaccine rates make new outbreaks of preventable diseases more likely.
These outsized public health challenges put strain on patients, but they also fall hard on nurses, pushing many nurses to the brink of exhaustion and to thoughts of leaving the profession.
And now President Donald Trump’s looming Medicaid cuts threaten to knock hundreds of thousands of North Carolinians off their insurance in the coming years and flood already crowded emergency rooms with patients who will no longer have access to primary care physicians.
Amid these overlapping challenges, North Carolina faces a nursing shortage that is projected to get much worse in the next decade.
“We do not have the workforce to meet the needs of the population,” Catherine Moore, a researcher at the Cecil G. Sheps Center for Health Services Research at UNC-Chapel Hill, told Cardinal & Pine.
“We have an aging population [as] nurses are retiring,” she said.
A 2021 Sheps Center study that looked at pre-COVID nursing trends in the state projected that North Carolina would face a nursing shortfall of 12,500 registered nurses by the year 2033. But the increased strain on nursing during the pandemic and its aftermath means a greater chance that nurses will retire early. With that variable added, the shortfall could nearly double, the Sheps center says.
RELATED: ‘We’re Drowning Out Here.’ NC Nurses Face Severe COVID Burnout
Moore’s colleague Erin Fraher presented this data to the General Assembly in 2022.
“I’ve never been so worried about a workforce in my life,” Fraher told lawmakers.
A recent proposal by the US Education Department could make it harder for the next generation of nurses as well, removing nurses from the recognized list of “professional degrees,” and limiting the amount a prospective nurse could get in student loans.
This rule could “create a barrier for many nurses seeking to advance their education, reduce access to patient care, and impact the stability of the nursing workforce,” the American Association of Colleges of Nursing (AACN) warns.
North Carolina is projected to have one of the largest nursing shortfalls in the country by 2035, the AACN says.
Unsafe staffing
Mission Hospital in Asheville, like many across the country, is severely understaffed, two Mission nurses recently told Cardinal & Pine.
According to a 2024 report by Wake Forest University, understaffing at Mission “caused a multi-faceted debacle” in the emergency room, increasing wait times and resulting in “an avalanche of complaints.”
RELATED: Mission Hospital nurses detail the ‘moral distress’ of working understaffed
But Mission is no outlier.
A 2022 study found that nearly 30% of nurses nationwide were considering leaving the profession, citing low pay, unsafe working conditions, and an unreasonable workload. These concerns were also the main points cited by New York City nurses when they went on strike this year, showing how little progress has been made in addressing the warnings nurses across the country have been sounding for years.
To keep nurses from leaving, some hospitals have been offering signing bonuses, with the average amount at about $20,000. According to a document obtained by Cardinal & Pine, Mission is now offering bonuses up to $50,000 for experienced nurses and $40,000 for recent graduates, with relocation bonuses up to $10,000.
Those numbers are huge. So is the need.
Mission needs 2,200 bedside nurses to safely staff the hospital, National Nurses United, the union that represents Mission nurses, said. As of August 2025, Mission had just 1,523.
Worse in rural areas
The need is even worse in rural areas, Moore said.
The number of nurses is actually growing in North Carolina, Moore said. But it’s not growing evenly.
“Registered nurses are more concentrated in urban areas of the state,” Moore said, and the workforce gap between cities and rural areas is widening.
The rate of registered nurses per population overall is 32% lower in rural areas than urban, according to the Sheps Center, and though the number of nurses in urban areas spiked shortly after the pandemic, it fell sharply in rural areas at nearly the same time.
And as Mission Hospital shows, staffing issues at a single hospital in rural areas can affect a huge swath of the population. Many communities have no Plan B when it comes to hospitals. Sicker patients mean overcrowded emergency rooms which mean more work for overworked nurses.
Long-term care facilities are also at risk
North Carolina is also expected to see a 30% shortfall in the number of licensed practical nurses (LPN) by 2033. LPNs have less training than registered nurses and their roles trend toward taking vital signs and samples and helping ensure a patient’s comfort, but they are still crucial parts of the healthcare infrastructure, Moore said.
“This workforce serves in our long-term care settings and they are also being used more in hospitals,” Moore said.
“I would be really concerned about the safety when you’re in a hospital or a long-term care facility or ambulatory care facilities, if they don’t have the workforce they need to take care of their patient load.”
Nurses are doing the best they can to take care of their patients, she said, but they still need the right support. Without it, their job gets harder.
“We’re all human,” she said. “If you don’t have the resources you need to do your work,” she added “mistakes get made.”
The next generation
The next generation is eager to join the fray, but there aren’t enough professors to teach them.
“A burnout crisis among bedside nurses combined with an existing shortage of nursing school faculty is putting unprecedented pressure on the current nursing workforce, exacerbating the situation,” The North Carolina Nurses Association said in a recent press release.
Being a doctor, being a nurse, saving lives, that’s hard work.
The next generation of medical experts are less likely to accept any conditions that make that work harder, Dr. Wes Wallace, an emergency room physician who also teaches at UNC, said.
“The term that’s heard more and more today: moral harm or moral hazard – that people just can’t take what’s asked of them,” Wallace said.
“We are clearly seeing that people from our medical schools are looking at that and saying, ‘Ah, gosh, I’m not sure that’s the way I wanna spend my professional career.’”
The stakes of the day-to-day professional lives of nurses and doctors are hard to imagine or quantify beyond the cliche: matters of life and death.
“We’re making tough decisions. We have to make them fast. Most of us work half of our shifts in the middle of the night, and that takes a toll physically, emotionally. We try to figure out smarter ways to do that,” Wallace said.
“But again, there’s a limit.”
Some action
Moore said that the Sheps Center presentation her colleague made to the General Assembly seemed to get lawmakers’ attention.
“I think that our state is trying to find some solutions,” she said.
“In the 2023/24 budget, the General Assembly actually passed legislation to increase the salaries of existing nursing faculty by up to 15%. And then for new faculty, to have an increase up to 10%,” she said.
Still, the solution has to mostly come from the hospitals and medical institutions themselves, Moore said.
Adequate staffing, safe-working conditions, and adequate pay are good for nurses, but they also speak to “the culture of the organization,” Moore said.
“Making sure that the nurses have good working conditions, resources to take care of their patients, feeling safe at work, having a healthy work-life balance, flexibility and support from their managers, ways of helping the staff themselves deal with stress, that all came out in the literature that we were able to find,” Moore said.
According to the managing consulting firm McKinsey & Company, 75% of the nurses who retired early in 2022 and 2023 cited feelings that their hospitals took advantage of them or did not value their work.
That stat, McKinsey said, is getting hospitals’ attention, and some are beginning efforts to improve conditions.
That would be great, Moore said.
“I want to learn more about what the employers are doing .. to keep their nursing staff, to keep all of their healthcare clinicians,” she said.
“It would be nice to hear more of that,” she said.
Support Our Cause
Thank you for taking the time to read our work. Before you go, we hope you'll consider supporting our values-driven journalism, which has always strived to make clear what's really at stake for North Carolinians and our future.
Since day one, our goal here at Cardinal & Pine has always been to empower people across the state with fact-based news and information. We believe that when people are armed with knowledge about what's happening in their local, state, and federal governments—including who is working on their behalf and who is actively trying to block efforts aimed at improving the daily lives of North Carolina families—they will be inspired to become civically engaged.


The Affordable Care Act turns 16, but the fight for affordable health care is far from over in NC
The ACA helped North Carolina expand Medicaid to more than 720,000 people, and prevented insurers from refusing to cover people with pre-existing...

Federal judge blocks HHS vaccine changes, citing a lack of scientific rigor
A US District Court sided with major medical institutions that the changes pushed by US Health Secretary Robert F. Kennedy Jr. were unlawful partly...

Medicaid helps keep this NC teen alive and at home. Trump’s health care cuts will put her at risk.
With $1 trillion in federal cuts to Medicaid looming and further cuts expected at the state level, the families of North Carolinians who rely on the...

Medicaid helps keep this NC teen alive and at home. Trump’s health care cuts will put her at risk.
With $1 trillion in federal cuts to Medicaid looming and further cuts expected at the state level, the families of North Carolinians who rely on the...
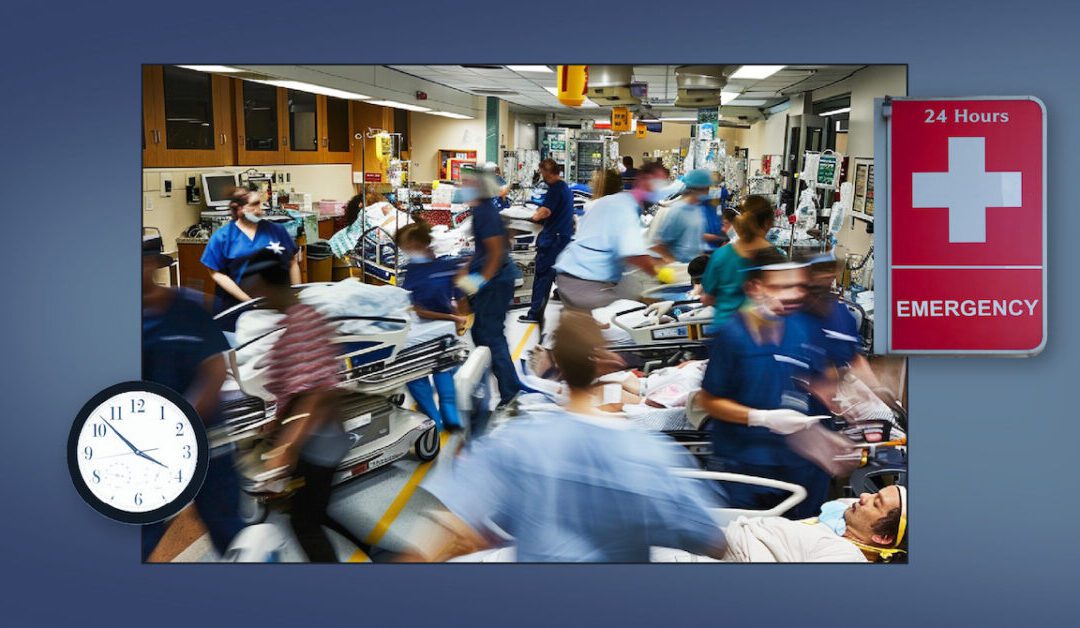
North Carolina’s ERs are already strained. Trump’s Medicaid cuts could make it worse.
When people lose insurance, they often rely on emergency rooms. But ERs were never intended to replace primary care, doctors warn North Carolina...





