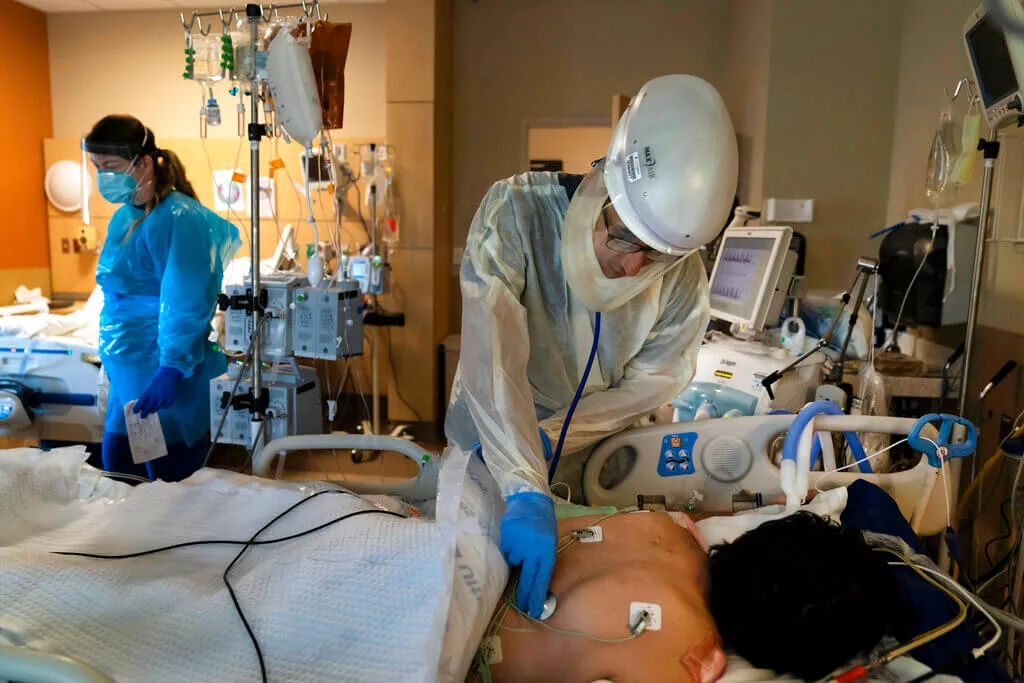
Hospitals across the country are on the brink of running out of space to treat COVID patients, which could lead to rationing care. (AP Photo/Jae C. Hong, File)
As space runs out in hospitals amid COVID’s worst surge yet, who receives treatment and who doesn’t could come down to healthcare systems that aren’t free of implicit bias.
As COVID-19 cases multiplied by 10, a Reno, Nevada hospital turned a parking garage into an ICU wing with 700 rapidly filling beds.
By Friday, the state of Mississippi did not have a single ICU bed available, forcing State Health Officer Dr. Thomas Dobbs to declare that all elective procedures requiring hospitalization must be delayed.
And in El Paso, Texas, an additional 10 morgue units and 1,500 medical professionals, plus both National Guardsmen and the incarcerated, were called upon to deal with the surge of infections and deaths from COVID-19.
Broadly speaking, the United States—while celebrating the first vaccinations against the coronavirus—is reaching a health care breaking point. Staffing shortages have also become a major concern, as hospital employees get sick or must undergo quarantine themselves.
Sorting Fact From Fiction: Sign up for the Cardinal & Pine newsletter.
“We may have enough ventilators but we may not have enough staff to operate those ventilators,” said Liz Sharlot, director of communications for the Mississippi health department.
“So, it’s a combination. There’s a lack of staff, a lack of hospital space.”
According to federal data, more than a third of Americans live in areas where hospitals are running critically short of intensive care beds, with one in 10 living in an area where intensive care beds are either completely full or less than 5% of beds are available. COVID-19 survival rates have improved since the start of the pandemic, as doctors have learned which treatments are more effective. However, the size of the current surge across the US means that shortages could nullify those gains, as healthcare workers must try to spread limited resources (including space and themselves) as far as possible.
With the current nationwide surge showing little sign of slowing, hospitals could soon institute crisis standards, which are guidelines for rationing health care. This means that more people could die as a result of not being able to directly receive the help they need at medical facilities. It also means that health practitioners are forced to decide who gets care, the level of care they receive, and who gets sent home.
Since September, the Centers for Disease Control and Prevention has tracked increasing levels of COVID infections, but the percentage of emergency department visits and hospital admissions for COVID-like illness has decreased slightly. “That suggests that there’s some rationing and stricter triage criteria about who gets admitted as hospitals remain full,” Thomas Tsai, an assistant professor of health policy at Harvard University, told The New York Times. Still, hospitalizations and mortalities for the most recent weeks are expected to increase as more data are collected.
RELATED: Only 6% of Med School Grads Are Black—Here’s Why That’s a Major Problem for the US
Over the summer, Arizona became the only state to officially activate crisis standards during their devastating surge. At the time, 91% of ICU beds and 85% of all hospital beds in the state were in use.
However, rationed care could become a reality in other parts of the country, where the need for care has grown beyond the means to treat patients.
The Idaho Board of Health and Welfare voted last week to finalize how the state’s “crisis standards of care,” a set of guidelines to determine how health care is rationed, would be activated. There, crisis standards apply beyond COVID patients, affecting everyone seeking medical attention at a hospital or similar facility, from car crash victims to flu patients. If a patient is deemed too likely to die, for example, they may not receive a ventilator immediately but could receive medication to reduce pain.
These standards of care also raise issues about equity within the healthcare system, particularly in light of studies demonstrating rampant implicit bias throughout the industry. Such biases can affect the way clinicians interact and communicate with Black or brown patients and lower the odds of a patient getting the level of medical care they need.
Disparities in who, exactly, work in the medical field also complicate matters. Studies show that racial concordance—when patients and physicians share the same race—leads to better communication and might improve the life expectancy gap between Black and white Americans by about 8%. However, the Association of American Medical Colleges found only 5% of American doctors identify as Black, and just under 6% as Hispanic or Latino.
READ MORE: Study: Contracting COVID Is ‘All About Where People Live. It Has Nothing To Do With Genes.’
These statistics are discouraging given the disproportionate instances of COVID infection and death among Black and brown communities across the country. And the likelihood of developing severe illness in those communities—a key determinant in how hospitals triage patients presenting with COVID-19—is equally determined by decades and centuries of social inequity.
At the moment—when life or death decisions related to who receives COVID care could soon be made in hospitals around the country—that is particularly alarming. According to Dr. Howard Koh, former Assistant Secretary of Health for the Department of Health and Human Services under President Obama, the disparities in COVID outcomes only highlight the underlying structural problems in the United States due to race. Those very same structures can play out in a system that hasn’t yet exorcised the demons of implicit bias.
“Studies have shown even the most well-intentioned physician or medical professional demonstrate unconscious bias in caring for others,” said Koh. “That’s why explicit and consistent training and education and commitment to cultural competence is absolutely critical for the future of our health care workforce.”
Politics

Op-ed: Michele Morrow poses a huge threat to NC public schools
Students with disabilities would particularly suffer if Michele Morrow were to become the state Superintendent of Public Instruction, Susan Book...

Biden makes 4 million more workers eligible for overtime pay
The Biden administration announced a new rule Tuesday to expand overtime pay for around 4 million lower-paid salaried employees nationwide. The...
Local News

VIDEO: Senate Republicans Block Bill to Extend Child Tax Credit
View this post on Instagram A post shared by Cardinal & Pine (@cardinalandpine) Monday was tax day, and Senate Republicans are...

The 5 most believable UFO sightings ever reported in North Carolina
Read about five alien encounters that may forever remain unexplained. When you think of the most common places where you might hear a UFO sighting...




